|
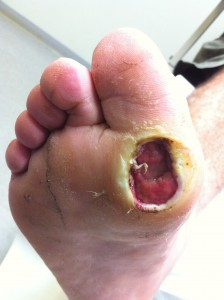
Diabetes mellitus (more commonly referred to as diabetes) is a disease in which an individual cannot secrete and/or utilize insulin for the breakdown of glucose [1]. This dilemma negatively affects the body’s ability to metabolize carbohydrates and other macronutrients [1]. Furthermore, diabetes also causes additional complications in the healing of wounds, as victims of the disease experience an overall hindered cellular and immune response as well as poor oxygenation and flow of blood at the wound-site [2]. The former impairs keratinocyte and fibroblast proliferation and movement and causes bacterial infection at the wound site [1-2]. Meanwhile, the latter generates a hypoxic environment which is never corrected via angiogenesis [2]. Additionally, reactive oxygen species (ROS) form as a result of hyperglycemia (due to poor insulin secretion and/or function) and these hypoxic conditions, ultimately delaying healing and promoting the breakdown of tissue [1-2]. Thus, while post-hemostatic wounds in healthy and non-diabetic individuals undergo inflammation and then smoothly and swiftly transition into epithelial cell proliferation and migration and tissue remodeling, diabetic wounds (such as a foot ulcers) are denoted by perpetual inflammation and the incomplete formation of new skin [1-4]. Figure 1 shows an example of a DFU [5]. To date, a clinical need still exists to create a solution for diabetic foot ulcers (DFUs) that simultaneously improves wound-site oxygen levels, neovascularization, angiogenesis, and keratinocyte and fibroblast proliferation and movement [1]. In the context of wounds, about 15% of diabetics will experience a DFU in their lifetime [3]. Most lower-leg amputation cases (84%) in diabetic patients involve such a wound occurring prior to the need and the performance of the operation [3]. Globally and as of 2010, diabetes affects approximately 285 million adults. By 2030, it is predicted that this population will increase by more than 54% [1]. Thus, until an adequate solution is developed, DFUs harm and will continue to impact a large and growing demographic. References
[1] L. I. F. Moura, A. M. A. Dias, E. Carvalho, and H. C. de Sousa, "Recent advances on the development of wound dressings for diabetic foot ulcer treatment—A review," Acta Biomaterialia, vol. 9, pp. 7093-7114, 7// 2013. [2] S. Guo and L. A. DiPietro, "Factors Affecting Wound Healing," Journal of Dental Research, vol. 89, pp. 219-229, 11/13/received 09/29/revised 10/30/accepted 2010. [3] H. Brem and M. Tomic-Canic, "Cellular and molecular basis of wound healing in diabetes," The Journal of Clinical Investigation, vol. 117, pp. 1219-1222, 2007/05/01. [4] R. G. Frykberg and J. Banks, "Challenges in the Treatment of Chronic Wounds," Advances in Wound Care, vol. 4, pp. 560-582, 01/23/received 05/04/accepted 2015. [5] The Chronic Pain Blog,. Diabetic Foot Ulcer. [Online]. Available: http://chronicpainblog.com/living-with-diabetic-foot-ulcers/. [Accessed: 27-Nov-2016].
0 Comments
|
|